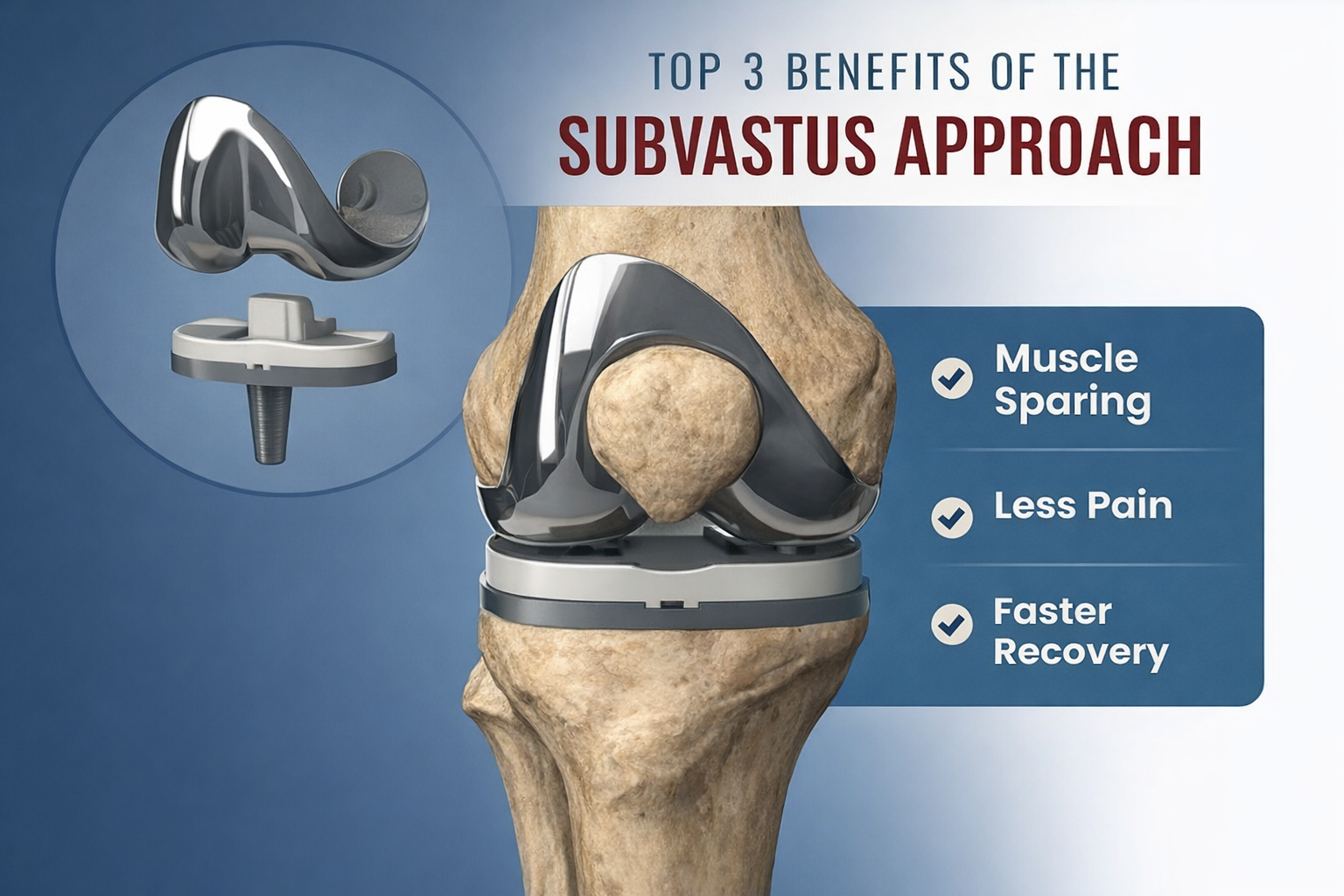
Standard Knee Replacement surgery Cuts Through Your Muscle.
Ours Doesn’t Have To.
The subvastus approach to knee replacement keeps your quadriceps intact — and science shows that changes everything about your recovery.
Find Out If You Qualify →*Data from peer-reviewed clinical trials. Individual results vary.
Most Patients Don’t Know There Are Two Very Different Ways to Do a Knee Replacement
If you or someone you know is facing total knee replacement (TKR), you’ve probably spent hours researching recovery timelines, implant brands, and physiotherapy. But there’s one question almost nobody asks their surgeon — yet it may be the single biggest factor in how quickly you get back on your feet:
“How exactly are you going to open my knee — and are you going to cut through my quadriceps muscle to do it?”
For over 90% of knee replacements performed worldwide, the answer has historically been: yes. The conventional “medial parapatellar” approach involves slicing through the quadriceps tendon — the powerful muscle group that lets you stand up from a chair, climb stairs, and walk without a limp. That cut heals. But it takes time. And during that time, you are weak, dependent, and in pain.
There is another way. And it’s called the subvastus approach.
What Is the Subvastus Approach?
The subvastus technique — sometimes called the “Southern approach” — is a surgical method for accessing the knee joint that goes beneath the vastus medialis muscle rather than through the quadriceps tendon. In plain language: the surgeon slides under the muscle instead of cutting through it.
The extensor mechanism — the entire chain of muscle, tendon, and soft tissue that powers your leg — is kept completely intact. The patella (kneecap) is gently moved aside, not flipped. The blood supply to the kneecap is preserved. And when you wake up from surgery, your quadriceps muscle has never been cut.
Your quadriceps is the most important muscle for knee function. Every day it remains uncut is a day closer to independence. The subvastus approach is specifically designed to protect that muscle — so your rehabilitation starts from a fundamentally stronger position.
The Clinical Evidence: What the Research Actually Shows
Thisnis not a gimmick. It is science. Multiple randomised controlled trials and meta-analyses have compared the subvastus approach to the standard medial parapatellar technique. Here is what the data consistently shows in the early and intermediate recovery phase:
| Recovery Outcome | Standard (Parapatellar) | Subvastus Approach |
|---|---|---|
| Straight leg raise achieved | Later (avg. 4 days slower) | Earlier ✓ |
| Day 1 pain score (VAS) | Higher | 0.8 pts lower on 10-pt scale ✓ |
| Range of motion at 1 week | Standard | 7° better ✓ |
| Painkiller use (week 1) | Standard | ~40% less ✓ |
| Lateral retinacular release needed | More frequent | 3× less likely ✓ |
| Quadriceps strength return | Slower | Faster ✓ |
| Long-term outcomes (1–10 yrs) | Equivalent | Equivalent |
A 2024 ten-year follow-up study confirmed what surgeons who use this technique already know: long-term outcomes are equivalent between both approaches — but the subvastus group reached functional milestones significantly faster in the critical early period, with lower pain scores and better quadriceps function at the one-year mark.
A comprehensive meta-analysis of nine randomised controlled trials (940 knee replacements) found the subvastus group scored significantly higher on the Knee Society Functional Score at 4–6 weeks and at 12 months — and needed lateral retinacular release three times less often, reducing surgical complexity and patellar complications.
The 5 Real Benefits for You as a Patient
Less pain from day one
An intact quadriceps means the muscle itself is not the source of your post-op pain. Patients consistently report lower pain scores on day one.
Walk and stand sooner
Patients who can straight leg raise earlier mobilise faster. This means shorter hospital stays and faster return to daily activities.
Stronger rehab start
When your quad is intact, rehab begins from a stronger baseline. You are rebuilding, not waiting for a cut tendon to heal before you can even begin.
Better patellar health
By preserving the medial blood supply to the kneecap, the subvastus technique significantly reduces risk of patellar avascular necrosis and subluxation.
Go home earlier
Multiple studies document shorter hospital stays with the subvastus technique — meaning less exposure to hospital-acquired complications and faster return to your own home.
No long-term compromise
At 1, 5, and 10-year follow-ups, subvastus outcomes match the standard approach — so you gain the early benefits without sacrificing long-term durability.
So Why Doesn’t Every Surgeon Use This Technique?
This is the question you deserve a straight answer to.
The subvastus approach requires greater surgical skill and experience. The exposure — the surgeon’s view of the knee joint — is more limited, especially in patients who are obese, have very stiff knees, or have had previous knee surgeries. Flipping the kneecap is harder. The operation typically takes 8–12 minutes longer.
For a surgeon who learned on the standard technique and performs it every week, switching approaches involves significant retraining. It is technically demanding in a way that rewards surgeons who have invested the time to master it.
This is not a criticism of the standard approach — it remains excellent, safe, and appropriate for many patients, particularly complex revision cases or severely deformed joints. But for straightforward primary knee replacement in appropriately selected patients, the subvastus approach offers a measurably better early recovery experience — and patients deserve to know that option exists.
“The best knee replacement is the one done by a surgeon who has mastered the approach — and chosen it specifically because it is right for you.”
Who Is a Good Candidate for the Subvastus Approach?
You are likely a strong candidate if:
- You are undergoing primary (first-time) total knee replacement
- You have moderate to good pre-operative quadriceps strength
- You do not have severe valgus (knock-knee) deformity requiring complex correction
- You have no prior major knee surgeries with significant scar tissue
- Your BMI does not severely restrict surgical exposure
Your orthopaedic surgeon will assess your specific anatomy, X-rays, and medical history to determine which approach gives you the best outcome.
Frequently Asked Questions
Ready to Walk Sooner After Knee Replacement?
Book a consultation to find out if the subvastus approach is right for your knee — and your life.
📞 Call Now WhatsApp UsMedical Disclaimer: This article is intended for general patient education only and does not constitute medical advice. Surgical approach selection is made by a qualified orthopaedic surgeon based on individual patient anatomy, medical history, and clinical judgment. All statistics cited are from peer-reviewed literature; individual outcomes may vary. Consult your orthopaedic surgeon for personalised guidance.
References
- Stubnya et al. Subvastus approach supporting fast-track TKA: network meta-analysis. J Arthroplasty, 2023. PubMed
- Migliorini et al. Better outcomes after mini-subvastus approach. Eur J Orthop Surg Traumatol, 2020. PubMed
- Teng et al. Subvastus vs parapatellar approach: meta-analysis. Orthopedics, 2012. PubMed
- EFORT Open Reviews. Subvastus vs parapatellar approach in TKA. 2018. Full Text
- Hosseini-Monfared et al. 10-year outcomes of subvastus vs standard approach. J Exp Orthop, 2024. PubMed
Dr Firoz Ahmed leading Orthopaedic Surgeon for Knee Replacement in Guwahati.
OPD Schedule: Mon – Sat (9AM to 4 PM)
Address: ARHI Hospital,11th Mile, Jorabat, Khanapara